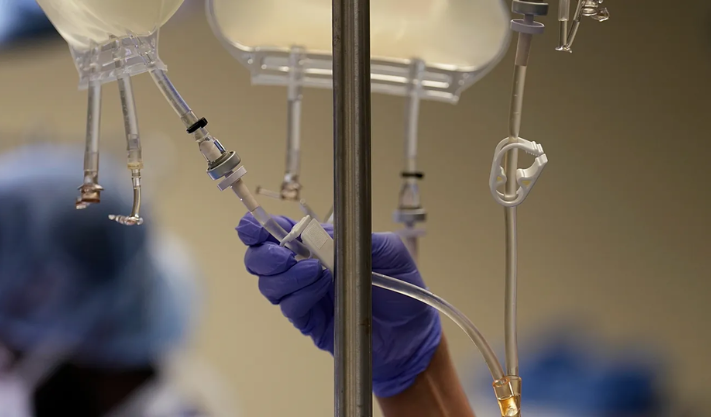
A System in Transition
State healthcare reform has become a defining issue in modern governance as policymakers work to ensure that healthcare systems are inclusive, affordable, and sustainable. With rising populations, increasing healthcare costs, and evolving medical needs, states are under pressure to rethink how care is delivered and financed. The primary goal of these reforms is clear: to broaden access to medical coverage so that no individual is left without essential healthcare services. This transformation reflects both a moral commitment and a strategic investment in long-term societal well-being.
Expanding Coverage to Underserved Populations
One of the central objectives of state healthcare reform is to include populations that have historically been excluded from formal healthcare systems. Low-income families, rural communities, and individuals working in informal sectors often lack access to insurance or affordable care. By expanding eligibility criteria and introducing subsidized programs, states aim to bring these groups into the healthcare fold. This approach not only improves health outcomes but also reduces the long-term costs associated with untreated conditions and emergency care.
Addressing the Affordability Challenge
Affordability remains a major barrier to accessing healthcare, even for those who have insurance. High premiums, deductibles, and out-of-pocket costs can discourage individuals from seeking timely treatment. State reforms tackle this issue through a variety of measures, including price regulation, financial subsidies, and cost-sharing mechanisms. These efforts are designed to ease the financial burden on individuals while maintaining the financial health of the healthcare system. Striking this balance is essential to ensuring that reforms are both effective and sustainable.
Strengthening Healthcare Infrastructure
Access to insurance alone is not enough if healthcare services are not physically available. Many regions, particularly rural and remote areas, suffer from inadequate infrastructure and a shortage of medical professionals. State governments are addressing this gap by investing in new hospitals, upgrading existing facilities, and providing incentives for healthcare workers to serve in underserved areas. These initiatives are critical to ensuring that expanded coverage translates into real access to care.
The Role of Technology in Healthcare Reform
Technology is playing an increasingly important role in reshaping healthcare systems. From electronic health records to telemedicine platforms, digital tools are improving efficiency and accessibility. Telemedicine, in particular, has emerged as a game-changer, allowing patients to consult doctors remotely and reducing the need for travel. Data-driven decision-making also enables states to allocate resources more effectively and design targeted interventions. By embracing technology, healthcare systems can become more responsive and patient-centered.
Emphasizing Preventive Care
Preventive care is a cornerstone of modern healthcare reform. Instead of focusing solely on treating illnesses, states are prioritizing measures that prevent diseases from occurring in the first place. Regular screenings, vaccinations, and health education campaigns play a vital role in this shift. Preventive care not only improves public health but also reduces the overall cost burden on healthcare systems. By addressing health issues early, states can create a more sustainable and efficient model of care.
Promoting Equity in Healthcare Access
Healthcare disparities often mirror broader social and economic inequalities. Factors such as income, geography, and education can significantly impact an individual’s ability to access care. State reforms aim to address these disparities by implementing targeted programs for vulnerable groups, including women, children, the elderly, and marginalized communities. Promoting equity ensures that healthcare systems serve all citizens fairly, regardless of their background or circumstances.
Public-Private Partnerships Driving Innovation
Collaboration between the public and private sectors is a key element of successful healthcare reform. Governments often partner with private insurers, healthcare providers, and non-profit organizations to expand coverage and improve service delivery. These partnerships bring additional resources, expertise, and innovation to the table. However, they also require strong regulatory frameworks to ensure that public interests are protected and that quality and accessibility remain top priorities.
Overcoming Financial and Administrative Challenges
Despite the progress made, state healthcare reform faces significant challenges. Funding remains a major concern, as expanding coverage and improving infrastructure require substantial investment. States must find sustainable financing solutions without placing excessive strain on taxpayers. Administrative complexities can also hinder the implementation of reforms, leading to inefficiencies and delays. Effective governance, transparency, and accountability are essential to overcoming these obstacles.
Navigating Political and Social Dynamics
Healthcare reform is often shaped by political and social factors. Differences in ideology, stakeholder interests, and public opinion can influence policy decisions and implementation strategies. Achieving consensus on healthcare reforms can be challenging, particularly in diverse societies. However, the universal importance of healthcare often drives policymakers to find common ground. Public awareness and engagement are also crucial, as informed citizens are more likely to support and benefit from reform initiatives.
Economic and Social Impact of Reform
The benefits of state healthcare reform extend beyond individual health outcomes. A strong healthcare system contributes to economic stability by reducing the financial burden of medical expenses and increasing workforce productivity. Healthy populations are better equipped to participate in education, employment, and community life. Additionally, improved healthcare access can foster social cohesion by reducing inequalities and promoting a sense of shared responsibility.
The Road Ahead: Building Resilient Systems
The future of state healthcare reform will depend on the ability of governments to adapt to changing needs and emerging challenges. Advances in medical technology, shifting demographics, and new health threats will require continuous innovation and flexibility. States must remain proactive, leveraging new tools and approaches to improve healthcare delivery. Collaboration across sectors and levels of government will be essential in building resilient and inclusive healthcare systems.
Conclusion: Toward Universal Access
State healthcare reform represents a comprehensive effort to broaden access to medical coverage and create a more equitable healthcare system. By addressing issues of affordability, infrastructure, technology, and equity, states are working to ensure that all citizens can receive the care they need. While challenges remain, the progress achieved so far demonstrates the potential of sustained and thoughtful reform. The ultimate goal is clear: a healthcare system that is accessible, affordable, and capable of improving the lives of everyone.
Also Read:-
What could drive markets this week? Key trends
US and Iran two-week truce eases rising tensions
Egg Prices Surge Across Europe Before Easter